
During my 8 years of incarceration, I experienced numerous lockdown events. It could be due to a fight in the yard or chow hall, an outbreak of an infectious disease like Norovirus, or a security sweep for weapons and contraband. It might last for a few hours to a few days. A security sweep might result in my property being tossed like a fruit salad onto my bed and my body strip searched, but that was the extent of my inconvenience. My few delayed meals or a sack lunch, a few missed shifts as a school tutor, canceled medical or library callouts, even a few missed visits do not begin to compare to what is happening now across the country. Lockdowns were just part of the prison experience, but that all changed with Covid-19.
My wife is a Medical Assistant and was hired during Covid to work in the state prison near our house. During the pandemic everything changed. Just like out in the world, prisons went into complete lockdown. No prisoner movement. What necessary minimal services like medical came to the housing units. All offsite prisoner transport stopped. No visits, no school or programing, no yard, weight pit of gym callouts, no church services or outside volunteers. Prisoners were not allowed to interact with other people from outside their housing units. The routine upon which prison is built was stopped completely. In most prisons this condition lasted not for a couple of months, but for over a year. In a previous blog post entitled Anti-Social Distancing I wrote about the devastating effects that the pandemic had on prisoners. The ripple effects of that time still reverberate in prisons.
In many U.S. prisons, “lockdown” no longer describes a rare emergency response to a riot or a narrowly targeted security incident. It has become a recurring operational mode: housing units sealed, movement halted, yard and dayroom time canceled, phones restricted, visits suspended, and education, treatment, and job assignments paused—sometimes for days, weeks, or even months. Reporting in recent years has documented extended lockdowns tied not only to violence but also to chronic understaffing and overcrowding, raising a stark question: When a prison can’t run its basic schedule safely, are we still operating a rehabilitative institution or merely warehousing human beings behind steel doors? [1]
What a Prison Lockdown Actually Means
Lockdowns vary by facility, custody level, and the event that triggered them. But in practice, a lockdown is a temporary suspension of normal movement and routines—often applied to an entire housing unit or whole prison—so staff can regain control, search for contraband, respond to violence, manage a shortage of officers, or contain disease outbreaks. Some lockdowns allow limited “controlled movement” (brief showers, medication lines, or staggered recreation). Others are near-total confinement to cell, with meals delivered to doors, minimal human contact, and sharply reduced access to healthcare, law library, religious services, and family contact.
Even when it is not formally “solitary confinement,” a prolonged lockdown can replicate many of the same risk factors: sensory deprivation, social isolation, loss of autonomy, and the collapse of predictable routines that help people regulate stress. That overlap matters because research on restrictive housing and solitary confinement consistently links extreme isolation to psychological deterioration, self-harm, and elevated suicide risk.
Mental Health: Why Lockdowns Hurt So Much
People enter prisons with high rates of mental illness and trauma histories, and many facilities already struggle to meet their clinical needs. The Prison Policy Initiative’s research library summarizes how common mental health diagnoses are in custody and how gaps in treatment persist. In that environment, lockdowns act like gasoline on a smoldering fire: they intensify stressors while simultaneously cutting off the very support: structured activity, social contact, counseling, movement, sunlight, and exercise that can keep symptoms from spiraling. [10]

- Loss of routine and control: Predictability is a core mental-health stabilizer. Lockdowns replace schedules with uncertainty—When will the door open? Will medication be on time? Will family calls work today?
- Isolation and conflict: Confinement increases loneliness and rumination, but it can also increase tension with cellmates in cramped spaces, producing hypervigilance and sleep disruption.
- Reduced physical activity: Yard closures and canceled recreation remove one of the most accessible mood regulators.
- Disrupted healthcare access: Even brief interruptions in psychiatric care, counseling, and medication continuity can trigger withdrawal, relapse, or acute crises.
- Family separation: Suspended visitation and restricted phone access remove a major buffer against despair—especially for parents.
We should be careful with language: lockdowns and solitary confinement are not identical. Still, a large body of evidence on solitary confinement provides a warning label for prolonged, near-total lockdown conditions. A major systematic review and meta-analysis in Frontiers in Psychiatry found solitary confinement was associated with adverse psychological effects and higher risks of self-harm and mortality, especially suicide. When whole housing units are kept in conditions that approximate isolation, it is reasonable to expect similar patterns—particularly among people with preexisting mental illness. [3]

Lockdowns also leave residue. After weeks of enforced inactivity, people may emerge dysregulated—more irritable, less trusting, and more prone to impulsive behavior. That dysregulation can feed a vicious loop: tension increases, violence increases, administrators respond with more lockdown, and the psychological and social environment degrades further. Meanwhile, the skills needed for successful reentry: emotion regulation, conflict resolution, consistent participation in treatment—are precisely the skills lockdowns erode.
Rehabilitation: Lockdowns Don’t Just Pause Programs—They Break Them
Education classes, vocational training, substance use treatment groups, cognitive behavioral programs, faith-based services, work assignments, and reentry planning often depend on predictable movement and staff availability. Lockdowns disrupt all of it. Even “temporary” cancellations can have outsized effects because correctional programming is built on momentum: attendance requirements, sequential curricula, waitlists, and limited seats. Miss enough sessions, and a person can lose their spot—then wait months to re-enroll, if they can at all.
This isn’t a minor inconvenience. Research syntheses and policy reviews consistently find that prison programming, especially education and job training, can reduce recidivism and improve post-release employment. RAND’s work on correctional education summarizes evidence that educating incarcerated people improves post-release outcomes, and federal reviews describe programming as a key lever for reducing reoffending. When lockdowns suspend programming, they effectively suspend one of the few tools’ prisons have to make future communities safer. [8] [9]

Lockdowns also damage the human infrastructure of rehabilitation: relationships. Family visitation is often suspended, and calls may be limited or unreliable. Staff may interact with incarcerated people primarily through orders and door slots. Over time, this can shift the culture from “managed community” toward “permanent crisis mode.” Recent accounts describe facilities held in extended lockdown conditions because agencies lack enough staff to safely run normal schedules—an operational failure with deep human costs.
Are Lockdowns Increasing? What U.S. Data Shows—and What It Doesn’t
If you’re looking for a single national dataset that tracks the frequency and duration of prison lockdowns across all U.S. state and federal facilities over decades, you’ll quickly hit a wall: lockdowns are not consistently defined, measured, or publicly reported across jurisdictions. National statistical agencies such as the Bureau of Justice Statistics (BJS) produce detailed annual reports on prison and jail populations, admissions, staffing, and mortality, but “lockdown-days per facility per year” is not a standard published metric. The Prison Policy Initiative even maintains resources explaining that many commonly requested criminal-justice datasets simply don’t exist in unified form—lockdowns being a prime example. [10] Here is one of the few examples from the Illinois Department of Corrections.
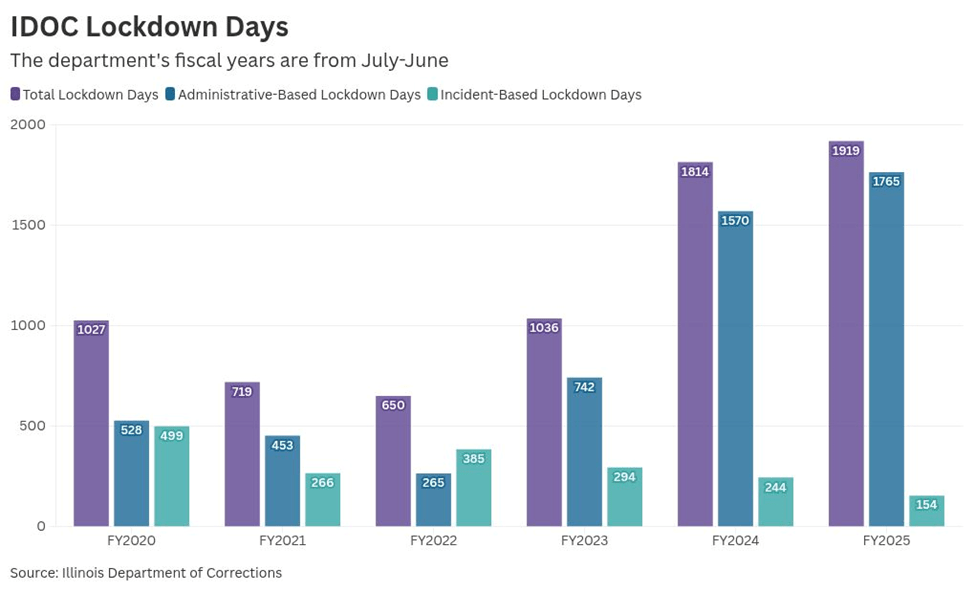
Still, we can responsibly analyze lockdown trends by triangulating from: (1) periods when lockdowns were system-wide (notably the COVID-19 era), (2) staffing and overcrowding indicators that predict operational lockdowns, and (3) investigative reporting and oversight findings documenting prolonged, non-emergency lockdown use. Note that throughout this article I have specifically included a series of images related to two state prisons in Wisconsin that made the news due to public protests regarding prolonged lockdowns and prison conditions.
1) The COVID-19 Shock: Lockdown as Public-Health Control
From March 2020 through early 2021, many prisons entered “modified operations” that resembled extended lockdowns: movement restrictions, suspended visitation, reduced programming, and quarantine/isolation practices. BJS documented the broader system impacts of the pandemic in prisons—including testing, infections, deaths, and major shifts in admissions and releases—showing how deeply COVID-19 altered daily operations behind bars. [4] Refer to my post Speech-less to read about the devastating effect that Covid-19 had on those incarcerated at that time.
Federal oversight also highlighted the mental-health danger of pandemic isolation. In a capstone review of the Federal Bureau of Prisons’ COVID-19 response, the DOJ Office of the Inspector General reported that the BOP told investigators that seven incarcerated people died by suicide from March 2020 through April 2021 while housed in single-cell confinement in quarantine units related to COVID-19—an alarming signal of how extreme isolation can interact with crisis stress. The OIG also described staffing shortages and morale challenges during the pandemic. [5]
At the time the BOP published facility-level COVID-19 statistics, which helped document disease burden and operational strain. That reporting was quickly ended even before the pandemic was declared over and the information was never translated into a standardized national ledger of lockdown frequency and duration.
2) The Staffing Squeeze: Lockdown as a Substitute for Adequate Operations
Outside of pandemic emergencies, one of the most commonly cited drivers of extended lockdowns is understaffing. When there aren’t enough officers to safely escort people to chow, yard, school, or the clinic, prisons cut movement. In its analysis of the national staffing crisis, the Prison Policy Initiative argues that understaffing becomes a self-reinforcing loop: fewer staff leads to more restrictive conditions and fewer services; conditions worsen; violence rises; staff burnout increases; recruitment becomes harder; and lockdown becomes routine. [2]

Data-driven reporting has underscored how severe the staffing decline has been. The Marshall Project reported that state correctional workforces dropped sharply after 2019, reaching the lowest mark in more than two decades in 2022, while many state prison populations began rebounding—creating a mismatch between staffing capacity and operational demands. In that context, lockdown becomes a predictable management response rather than an exceptional security measure. [6]
Stateline’s national reporting similarly describes prolonged lockdowns, sometimes lasting weeks or months—linked to understaffing and overcrowding, not disciplinary need. The key trend described is not necessarily “more lockdown events,” but longer lockdowns and more frequent reliance on lockdown-like restrictions as a default operating posture. [1]

3) Security Threats: Contraband, Drugs, Phones, and Violence
Lockdowns are also frequently used after violent incidents, when administrators suspect weapons, or when contraband flows overwhelm routine searches. A National Institute of Justice summary of a RAND-facilitated workshop on correctional security threats ranked insufficient staffing as the top concern among experts, with contraband (drugs, weapons, cellphones) generating the largest number of priority needs. Each of these threats can precipitate facility-wide shakedowns and movement freezes, especially when an agency lacks the personnel and technology to target responses precisely. [7]
So, are lockdowns increasing? We cannot prove a clean nationwide time-series increase in lockdown frequency and duration because the U.S. lacks standardized, publicly reported lockdown metrics across prisons. But multiple converging indicators suggest a real shift toward more extended lockdown conditions since 2020: pandemic-era modified operations, followed by persistent staffing shortages and overcrowding pressures that make normal programming schedules difficult to sustain. The lived reality described by oversight bodies and national reporting is consistent with longer and more routine restrictions—even if the number of discrete “lockdown events” is not measured uniformly.
Underlying Causes: Why Lockdowns Keep Spreading
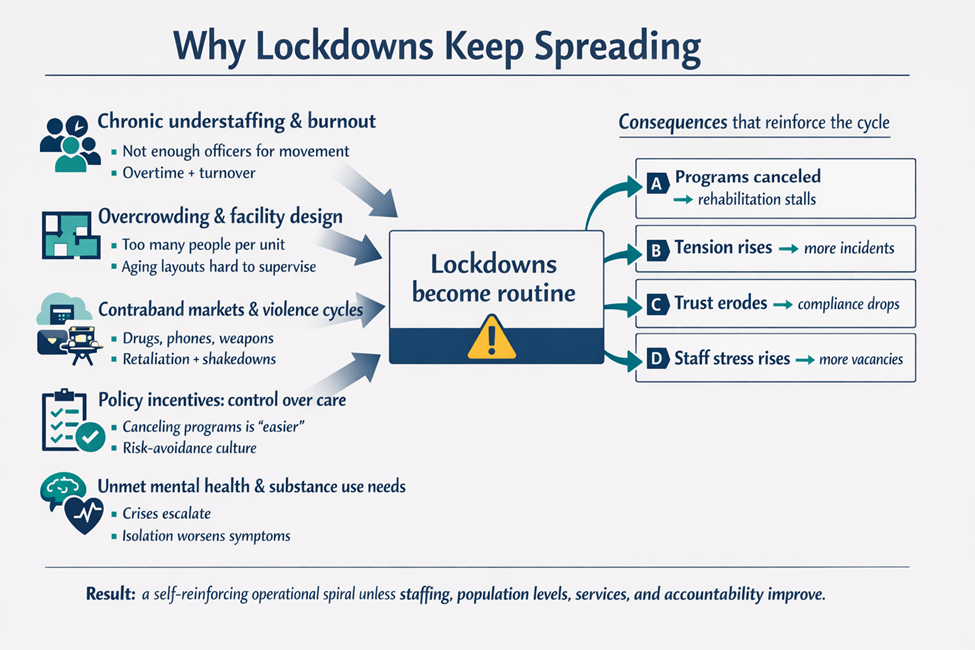
- Chronic understaffing and burnout: When posts go unfilled and overtime becomes constant, prisons cannot safely move large groups. Lockdown becomes the operational workaround. [1] [2] [6]
- Overcrowding and facility design: Crowded units, dorm settings, and aging infrastructure make it harder to separate conflicts, quarantine illness, or run staggered movement without enormous staffing. [1]
- Contraband markets and violence cycles: Illicit phones, drugs (including opioids), and weapons drive shakedowns and retaliatory violence, often followed by facility-wide lockdown. [7]
- Policy incentives that favor control over care: It is administratively easier to cancel activities than to build staffing, training, clinical capacity, and targeted security approaches.
- Unmet mental health and substance use needs: When treatment access is thin, crises escalate; crises prompt lockdowns; lockdowns worsen mental health; and the cycle continues. [3] [10]

What Can Be Done: A Humane, Evidence-Based Path Out of the Lockdown Spiral
Calling this a “humanitarian crisis” is not hyperbole: prolonged, population-wide confinement in stressful environments predictably harms mental health and sabotages rehabilitation. The good news is that the solutions are not mysterious. They require political will, operational discipline, and transparency.
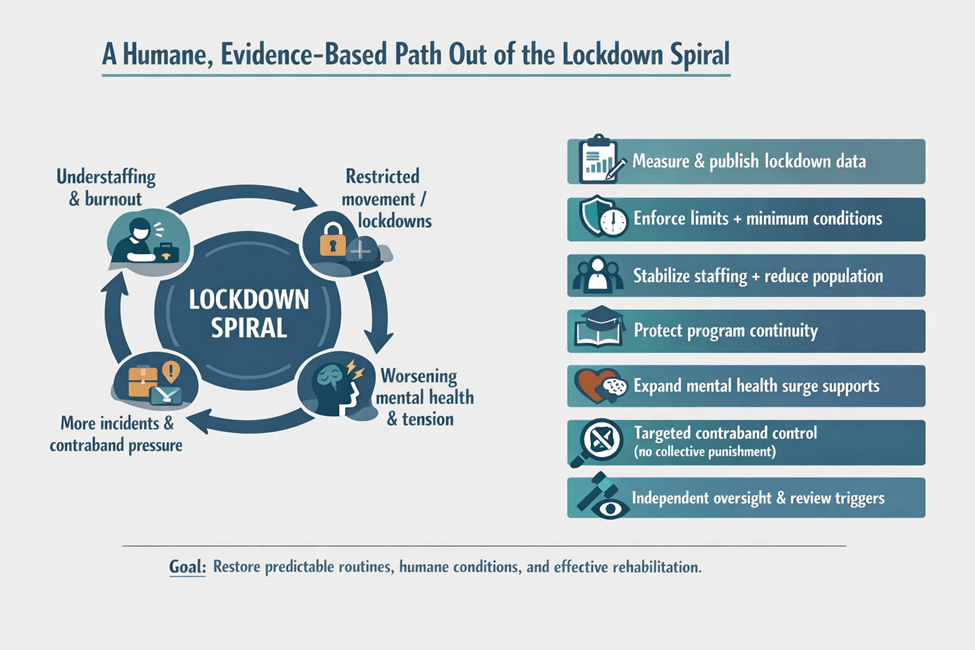
- Measure lockdowns—then publish the numbers. States and the federal system should track at minimum: lockdown start/end times, scope (unit vs. facility), reason codes, services suspended, and out-of-cell hours provided. Without data, the public can’t distinguish emergency necessity from routine deprivation. (The current lack of standardized lockdown metrics is a central barrier to trend analysis.) [10]
- Set enforceable limits and minimum conditions. Even during lockdowns, people should receive daily out-of-cell time, access to showers, medical and mental health care, and meaningful communication with counsel and family, with clear exceptions only for immediate, documented threats.
- Stabilize staffing—but don’t pretend hiring alone can solve mass incarceration. The staffing crisis is real, but it is tightly linked to the scale of incarceration. Breaking the cycle means improving working conditions (training, safety, schedules, pay) while also reducing the incarcerated population so staffing ratios are feasible. [2] [6]
- Protect program continuity as a public-safety priority. If education and treatment reduce recidivism, then suspending them for long periods should be treated as a risk to community safety. Build “lockdown-resilient” programming: cell-front coursework, tablet-based learning (where feasible), small-group controlled movement, and make-up sessions that prevent people from losing their place in sequenced programs. [8] [9]
- Expand mental health support during and after lockdown periods. Lockdowns are predictable stress spikes. Facilities should implement surge mental-health checks, peer-support access, and rapid referral pathways during restrictions, especially for people with known risk factors for self-harm. The evidence linking extreme isolation to self-harm and suicide risk makes this essential. [3] [5]
- Modernize contraband control without collective punishment. Targeted searches, intelligence-led investigations, and technologies aimed at drones and illicit phones can reduce the perceived need for sweeping lockdowns—while still addressing the very real threats highlighted by correctional security experts. [7]
- Strengthen independent oversight. Prolonged lockdowns should trigger automatic external review: documentation of necessity, timeline for restoration of normal operations, and a plan for services. Oversight findings during COVID-19 show why independent scrutiny matters. [4] [5]
Conclusion: Safety Without Humanity Isn’t Safety
Lockdowns will always exist in some form; prisons are volatile places, and emergencies happen. The crisis is the normalization of lockdown as routine management, whether driven by pandemic protocols, staffing collapse, overcrowding, contraband economies, or a deeper policy choice to prioritize control over care. The mental-health consequences are predictable, and the rehabilitation costs are measurable in missed education, stalled treatment, and weakened family ties.
Because the United States does not systematically publish lockdown frequency and duration data across jurisdictions, we can’t chart a definitive national curve the way we can for incarceration rates or admissions. But the available evidence strongly suggests the experience of lockdown has intensified since 2020; first through widespread pandemic restrictions documented by BJS and federal oversight, then through persistent staffing and capacity failures that keep prisons from operating normally. Treating this as a humanitarian crisis starts with telling the truth in numbers: track lockdown-days, publish them, and make “days of life” behind bars a metric of accountability alongside safety. [4] [5] [1] [2] [10]
Endnotes
- Stateline. Amanda Hernández (December 3, 2024). “State prisons turn to extended lockdowns amid staffing shortages, overcrowding.”
- Prison Policy Initiative. Brian Nam-Sonenstein & Emmett Sanders (December 9, 2024). “Why jails and prisons can’t recruit their way out of the understaffing crisis.”
- Luigi, M., Dellazizzo, L., Giguère, C.-É., Goulet, M.-H., & Dumais, A. (2020). “Shedding Light on ‘the Hole’: A Systematic Review and Meta-Analysis on Adverse Psychological Effects and Mortality Following Solitary Confinement in Correctional Settings.” Frontiers in Psychiatry, 11:840.
- U.S. Bureau of Justice Statistics. Carson, E. Ann; Nadel, Melissa; & Gaes, Gerry (August 2022; published August 25, 2022). Impact of COVID-19 on State and Federal Prisons, March 2020–February 2021 (NCJ 304500).
- U.S. Department of Justice, Office of the Inspector General (March 2023). Capstone Review of the Federal Bureau of Prisons’ Response to the Coronavirus Disease 2019 Pandemic (Report 23-054).
- The Marshall Project. Shannon Heffernan & Weihua Li (January 10, 2024). “New Data Shows How Dire the Prison Staffing Shortage Really Is.”
- National Institute of Justice (April 6, 2020). “Experts Identify Priority Needs for Addressing Correctional Agency Security Threats.”
- RAND Corporation. Davis, L. M., Bozick, R., Steele, J. L., Saunders, J., & Miles, J. N. V. (2013). Evaluating the Effectiveness of Correctional Education: A Meta-Analysis of Programs That Provide Education to Incarcerated Adults (RR-266).
- Office of Justice Programs / Federal Probation. Byrne, J. M. (2020/2022). “The Effectiveness of Prison Programming: A Review of the Research Literature Examining the Impact of Federal, State, and Local Inmate Programming on Post-Release Recidivism.”
- Prison Policy Initiative. “Data toolbox” (includes guidance and a list of commonly requested data that doesn’t exist in unified form).
